Visceral leishmaniasis, known in India as kala-azar or black fever, is a parasitic disease that kills an estimated 500,000 people a year, 90 percent of them in India, Nepal, Bangladesh, Brazil and Sudan.
In India, the disease is endemic in the northeastern Indian State of Bihar – the epicenter of kala-azar in the region – and in Jharkhand, Uttar Pradesh and West Bengal. It manifests with irregular bouts of fever, substantial weight loss, swelling of the spleen and liver, and anemia. Left untreated, kala-azar is almost always fatal, especially in children,
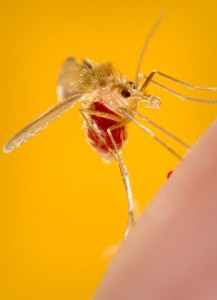
Photo Credit: James Gathany, Centers for Disease Control and Prevention.
According to the World Health Organization (WHO), “Leishmaniasis is a poverty-related disease. It affects the poorest of the poor and is associated with malnutrition, displacement, poor housing, illiteracy, gender discrimination, weakness of the immune system and lack of resources. Leishmaniasis is also linked to environmental changes such as deforestation, building of dams, new irrigation schemes and urbanization, and the accompanying migration of non-immune people to endemic areas.”
Leishmania, the protozoan parasite that causes kala-azar, spreads to humans through the bite of infected female sandflies.
The sandfly bite causes tissue damage that, although minimal, promotes recruitment of neutrophils to the site of injury. Neutrophils are powerful phagocytic cells that participate in the primary immune defense mechanism of the host. However, neutrophils are also the primary target of leishmania — the parasite is not killed by the neutrophils — rather, the parasite survives within them until the neutrophils are engulfed by macrophages. Leishmania is not even killed during this step of the immune response — instead, it survives and multiplies inside the macrophages. There, it modulates the normal defense mechanisms, it increases the membrane fluidity of the macrophages and disrupts lipid rafts, thus impairing their ability to present the antigen. Thus, Leishmania starts a process that hijacks the entire immune system for its survival.
No vaccine has yet been licensed to prevent infection.
Drugs to treat the disease are toxic and expensive. In Bihar, where 90% of India’s large kala-hazar burden is located, the parasite has developed resistance to one of the main treatments, a group of drugs known as antimonial preparations. Indeed, the effectiveness of the antimonial preparations is now so low that these drugs are no longer recommended in the Indian subcontinent, whereas they remain an essential part of the treatment for visceral leishmaniasis in South America and sub-Saharan Africa.
Researchers at the Universities of Dundee and Aberdeen in the U.K. report, in an article published in the journal Proceedings of the National Academy of Sciences of the United States of America, that arsenic contamination of the water supply may have played a significant role in building the resistance of leishmania to the antimonial drugs.
In the article, the researchers state: “The Indian subcontinent is the only region where arsenic contamination of drinking water coexists with widespread resistance to antimonial drugs that are used to treat the parasitic disease visceral leishmaniasis.” The article (October 28, 2013) is titled “Chronic exposure to arsenic in drinking water can lead to resistance to antimonial drugs in a mouse model of visceral leishmaniasis”
Professor Alan Fairlamb, senior author of the article, said: ”The water supply in Bihar has been found to be affected by contamination from naturally occurring arsenic in the groundwater. What we have been able to show through experiments is that arsenic contamination of water can build resistance in Leishmania parasites to antimonial treatments.”
The researchers performed their experiments in animals. They serially passaged the leishmania parasites in mice. During the passages, mice received arsenic in drinking water at environmentally relevant levels. Results from these experiments show that after five monthly passages, the leishmania parasites become stably resistant to an antimonial preparation.
Meghan Perry, lead author of the study, said: “Arsenic contamination of the groundwater is a serious issue in Bihar. Many villagers continue to drink arsenic contaminated water as they have no alternative. Knowledge of the dangers of arsenic pollution is low and mitigation projects are not reaching all of those in need. Arsenic can lead to a myriad of health issues and our research adds to this long list. Community education and alternative drinking water sources are desperately needed.”
This new study points out an additional detrimental effect of arsenic in drinking water. Another example of adverse effect mediated by arsenic and recently demonstrated is the increase in respiratory diseases following fetal exposure.

When diseases arise, many assume that the best course of action is to develop a pharmaceutical drug or vaccine to treat or prevent infection. Developing these treatments can be tedious, and administering them to developing countries can be expensive or inconvenient. However, there are alternate methods to reduce the spread of a disease. One way is by attacking the source. In this case, fighting off the insects could be a worthy area of focus in reducing incidence of kala-azar.
It states above that female sandflies spread the protozoan parasite. Malaria is another well-known disease that is also caused by a protozoan, and spread by mosquitoes. A fairly recent procedure, the sterile insect technique, is still in development. It is a method of controlling insect populations by introducing sterile insects into the environment. Since many parasitic insects that bite humans are female, sterile males would compete with wild males for females, and result in reduced offspring (1). This is how geneticists can make an impact on disease-prevention. If scientists can successfully sterilize populations of these insects and introduce them to the environment, it would help reduce cases of these parasitic diseases.
References:
1) Dyck, V.A.; Hendrichs, J.; Robinson, A.S., eds. (2005). Sterile Insect Technique: Principles and Practice in Area-Wide Integrated Pest Management. Dordrecht, The Netherlands: Springer.
I agree that attacking the source of the problem would provide a better alternate method to reduce the spread of disease, but I don’t think using the sterile insect technique would be as applicable as it may seem, especially in nature. I do understand the reasoning behind why sterilizing populations of insects can reduce the cases of parasitic diseases, but what are the chances of this method actually being successful? If sterile male sandflies were introduced into the population, what guarantees their success in outcompeting the wild males for females? Scientists would probably have to modify a few genes to ensure that these sterile males beat other males. These genes can be those that affect size (making them larger) or wing span (making them better fliers) – anything that can give them that competitive edge over their counterparts. If they don’t, I don’t see how sterile males can naturally beat the wild types to gain access to mates. There’s also the possibility that females may not mate with these sterile males because there’s a reproductive disadvantage. Female flies, like many other types of animals, are mainly concerned about producing offspring for the next generation, passing on her genes. If mating with sterile males produces no offspring, female flies will likely develop a bias against males who are sterile. She will avoid those that will not benefit her, creating a disadvantage for those sterile males. These are just some of the reasons why I think the sterile insect technique may not work.
If we can’t reduce the number of infected flies, or eliminate the parasite itself (since antimonial preparations aren’t working), we can do something about the arsenic levels in the water by raising awareness. If more people knew about this problem, perhaps more can be done to provide these infected areas with the resources needed to clean their water supply.
I actually think that the proposed sterile insect technique could actually work. They would surely be tested for effectiveness (eg. seeing whether or not the females will mate with them, and whether they could out-do the wild males) before being sent out. So, I don’t think that’s a big concern. Scientists could alter them to make them as effective as they need, and after a few attempts I think it would work just fine. And, while it may not completely get rid of the sandfly, it would greatly reduce their number, allowing for some relief in the endemic areas.
You also proposed that we should clean the water supply in the greatly affected areas. Although this is something that should be done anyway, to prevent illness and diseases of various types, I don’t think it would be effective in this case. The article points out the presence of arsenic in the water supply may have led to the the Leishmania becoming resistant to treatments that once worked. Thus, the harm has been done. Cleaning the water supply won’t undo that resistance of the protozoan, or anything else beneficial in the case of Leishmania. And this is why the sterile insect technique seems promising. It avoids drugs altogether and attacks the problem from a different angle.
This doesn’t surprise me in the least since arsenic is known to cause all sorts of problems in the human body. For the sandfly problem in those areas, perhaps a cheaper more efficient type of insect repellant that has DEET in it, can be manufactured. If it was distributed to people in those areas, perhaps they can put it on themselves and their children when they’re around water sources, to avoid the insect bites that lead to Visceral leishmaniasis. The problem with that is, the sandflies could either become resistant to this repellent or it would just be too costly for the poor areas most affected. So something should definitely be done about these sandflies, it wouldn’t hurt to try the sandfly male sterilization and possibly solve the problem from the root. The only problem with that is, these protozoans tend to find a way to survive regardless. So even with sterilization, who knows what could arise later.
In regards to the arsenic contamination of the water supply affecting the treatment of antimonial compounds in people, I have found instances where another drug is used and is just as affective against the disease. In a study done in Columbia where two individuals were actually found to be resistant against the antimonial drug, Liposomal amphotericin B was used instead (2). It proved to have a shorter time for treatment and was cost-efficient since the hospital stay doesn’t need to last as long. The only thing that needs to be monitored while administrating this drug, is renal function because amphotericin B tends to cause renal toxicity in people (1). Even with this back up medication, the underlying problem is the arsenic in the water supplies that are causing more harm than just resistance against antimonial compounds. I have read about a subterranean arsenic removal (SAR) technology that doesn’t use any chemicals at all, and produces no sludge and is actually done by controlled oxidation (3). Some countries are installing it for filtration of arsenic from drinking water and I think it would be a great project to install in rural areas in India. It would be a project worth developing by the government there, no matter the cost, since it’s causing serious problems all over India, including these new finding on arsenic’s affect on this drug. If arsenic could cause resistance with antimonial drugs, then it must be causing other issues as well.
1. http://www.sciencedirect.com/science/article/pii/S0924857904003498
2. http://www.ncbi.nlm.nih.gov/pubmed/19739006
3.http://www.insituarsenic.org/
I think that treating poverty stricken populations with chemical insect repellents is just as harmful as it is potentially beneficial. These populations not only source their drinking supply from natural water sources but also use them for hygiene and negatively are also contaminated with sewage runoff. I feel like even more fortunate populations are not fully aware of the proper use of repellants containing deet. Although deet is an effective prevention technique for repelling many disease carrying insects, if ingested deet can cause many problems internally including a variety of detriment from nausea and gastrointestinal issues to more severe neurological complications. If these populations are drinking the same water that they are using to bathe in, the deet repellants that would be topically applied would contaminate the water source. Combined with the numerous complications that arsenic contamination causes by itself these two could be a deadly dynamic duo.
I like the idea of discovering new vaccines that are not affected by arsenic as previously mentioned. The more that I think about this being a possibility, I also try to better understand why such options haven’t been an option before. I think the most important topic is understanding the mechanisms that are involved in leishmania parasite invasion. If they are target neutrophils, and the neutrophils are not having an effect on their destruction, I ponder the missing link. The ADCC (antibody-dependent cell-mediated cytotoxicity ) explains how neutrophils rely on other antibodies in the system to be activated. If these antibodies aren’t present, the Fc receptors on the surface of the neutrophils have nowhere to attach. Parasites are more complex in structure than bacteria and that alone could play a role in antibodies being expressed on their surface that would activate neutrophils.
I think there are many ways that this could be explained and that many have been explored. I feel like combining these ideas may lead to more successful breakthroughs in treatment for this ongoing problem.