During the past year, Zika virus has been moving north from Brazil into the Caribbean—bringing along several cases of microcephaly, a genetic defect characterized by small heads and brain damage in newborns. Indeed, infections caused by Zika virus are linked to microcephaly in children born to infected mothers, and to Guillain-Barré syndrome, a form of temporary paralysis, in adults. While most people recover from Guillain-Barré syndrome, some have permanent damage. In rare cases, Guillain-Barré syndrome leads to death. Zika, like Chikungunya and Dengue, is spread by the bite of an infected mosquito. However, cases of sexual transmission have been reported in several countries.
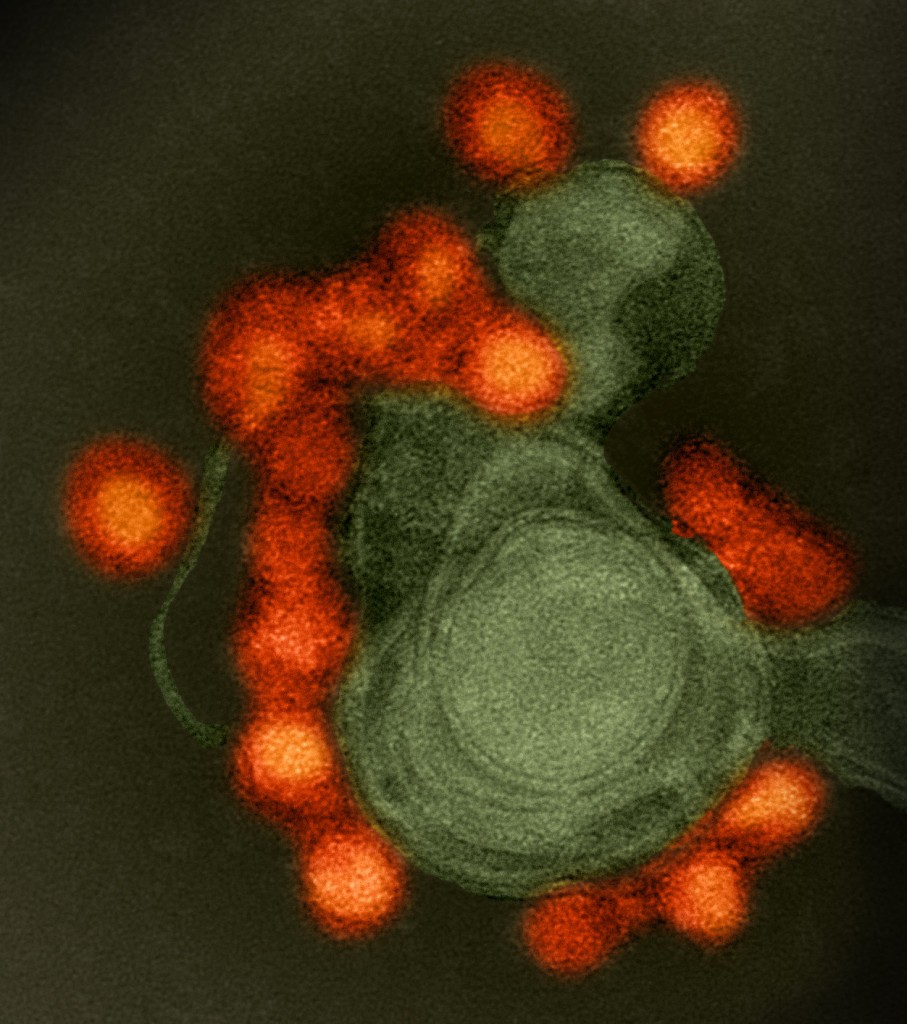
On February 1, 2016, the World Health Organization (WHO) declared “that the recent cluster of microcephaly cases and other neurological disorders reported in Brazil, following a similar cluster in French Polynesia in 2014, constitutes a Public Health Emergency of International Concern.”
The WHO expects the virus to spread from northern Argentina to the southern United States by the end of the year, infecting many millions of people. There is no vaccine against the Zika virus. Not surprisingly, scientists are racing to develop one.
The National Institute of Allergy and Infectious Diseases (NIAID), National Institutes of Health, is actively pursuing multiple vaccine candidates to prevent Zika virus infection, including:
- A DNA-based vaccine that uses a strategy similar to an investigational flavivirus vaccine for West Nile virus infection. That vaccine, which was developed by scientists at the NIAID Vaccine Research Center, was found to be safe and induced an immune response when tested in a Phase 1 clinical trial.
- A live-attenuated (live but weakened virus, so that it cannot cause disease) investigational Zika vaccine building on a similar vaccine approach for the closely-related dengue virus. The dengue vaccine candidate was shown to be safe and immunogenic in early-phase trials, and is currently being evaluated in a large Phase III study in Brazil.
- An investigational Zika vaccine that uses a genetically engineered version of vesicular stomatitis virus—an animal virus that primarily affects cattle. VSV was successfully used in an investigational Ebola vaccine tested by NIAID. This vaccine approach is at an early stage with plans underway to evaluate the Zika vaccine candidate in tissue culture and animal models.
- A whole-particle inactivated Zika vaccine based on a similar vaccine approach used by the Walter Reed Army Institute of Research (WRAIR) to develop vaccines against the related Japanese Encephalitis and dengue viruses.
Anthony Fauci, NIAID Director, said there are plans to begin testing a vaccine in 80 people in September 2016. This early-stage trial would examine whether an experimental vaccine is safe and generates immune responses in vaccinated volunteers. Fauci said that if the vaccine proves safe and capable of stimulating relevant immune responses, NIAID will launch in the first quarter of 2017 a phase 2b study in a country that has a very high rate of infection. That study would enroll thousands of volunteers. “If in the early part of 2017 we still have major outbreaks in South America and in the Caribbean, we may show that it’s effective or not within a year,” Fauci said.
However, a safe, effective, fully licensed Zika vaccine will likely not be available for several years.

Zika virus was first reported in 1947, and at that time, Zika fever was the most common illness caused by Zika virus, of which the infected person had no symptoms or mild symptoms. But nowadays, especially started from last year, Zika virus has become a raising problem around the world.
I am really interested in diagnosis of Zika virus infection. I know that one of the ways to inspect the infections of pregnant women is to look for symptoms such as fever, rash, joint pain or red eyes. If the woman has those symptoms and went to the areas invaded by the Zika virus, she may be infected by Zika virus. what if the infected pregnant woman did not show any symptoms? In this case, I think the diagnosis of Zika virus is extremely important to prevent the infected pregnant woman from giving birth to a baby with microcephaly. According to the CDC, they began to use anti-Zika IgM ELISA testing to diagnose the Zika virus infection. Anti-Zika IgM ELISA is an appropriate serodiagnosis method of acute Zika virus infections by testing human antibodies. The plate in ELISA was coated with virus-specific recombinant non-structural protein (NS1), so scientists can avoid cross reaction. Therefore, it would be easier to distinguish the Zika virus infection and dengue infections, which share the similar symptoms. And the acute infections are indicated by the virus-specific IgM antibodies or increased number of IgG in the serum. For the first step in ELISA, diluted human samples are added to the wells and incubated. If there are antibodies specific to this antigen, they will bind to them. After that, anti-human IgM with enzyme label will be added to the wells and bind to the primary antibodies. The positive results will be suggested by the color development.
I am glad to see there are platforms for hunting the Zika virus vaccines. Not having vaccines to a life-threatening viral disease is similar to not having antibiotics to superbugs. Making the vaccines is as important as diagnosis the infections. And I am looking forward to seeing the results of testing vaccines in September 2016.
With the current race to develop a Zika virus vaccine, I can’t help but wonder how the virus will evolve over the next ‘several years’. Given the evolution of viruses, what if the vaccine is not even effective in several years? Also, is there any program put in place by the CDC, FDA, or any agency in the US that allows for rapid clinical trial progression if the threat is spreading so quickly?
I understand that cultivating a vaccine is a gigantic undertaking that takes a lot of time to perfect, but is there another way? Is there anything that we can do in the meantime to prevent the spread of the virus?
It turns out that Julia Hilliard of Georgia State University is currently working on developing an antiviral drug to help slow down the spread of viruses in a local population during an outbreak. When tested on animals given the drug orally, the viral load was notably reduced and prevented death from the disease. Dr. Hilliard specializes in zoonotic viruses among many other pathogenesic organisms, and through her research she discovered that viruses block type-1 interferons. With this new knowledge, she aims to interrupt the virus pathways and prevent infection. I have high hopes for the research of our fellow Eagle and commend her for her progress thus far. Dr. Hilliards research could be a major player in the prevention of diseases caused by viruses.
The question as to whether the genetic mutation of Zika virus would render any current vaccine development ineffective is a valid one. It is true that vaccinations are developed and formulated based on the current molecular structure of the target and any change in that molecular structure can alter the efficacy of the drug. However, as science has shown, it takes a long period of time for a virus to mutate and, as such, research conducted today to develop a vaccine against Zika can remain effective for several years. In the future, perhaps research and technology can advance to the degree where, as genetic mutations occur, the vaccinations can be adjusted to respond accordingly.
To your other point, I agree with your concerns regarding an alternative approach to the situation, such as halting the spread of the disease. Zika virus has become a pandemic and should warrant a “State of Emergency” reply by the government, which could fund a “rapid clinical trial progression” or other aggressive testing given the extreme and widespread outbreaks reported.
Could there be a possible prophylaxis to prevent women from contracting Zika virus and causing microcephaly in their children? Yes, birth control. It would be very difficult to regulate international traveling, and most travelers engage in sexual intercourse in their normal day lives. Travelers that travel to areas with Zika might not always use contraceptives, and this risky behavior can lead to unplanned pregnancies. Since there is no way to temporarily band sexual intercourse in travelers that traveled to Zika areas, doctors can prescribe birth control medication as a prophylaxis to prevent microcephaly in unplanned pregnancies. The New York Times reports El Salvador has advised women not to get pregnant for the next two years since there is no available vaccine against the Zika virus. Instead of trying to regulate traveling, sexual intercourse, or pregnancies we have to inform travelers of the risks and prescribe any medication that can help decrease the disease symptoms until the vaccine is developed.
I agree there should be preventative measures that take place to prevent women who are in their child-bearing years from contracting Zika virus and their fetus being affected. Definitely increasing sexual health awareness, pushing for it in the countries affected by Zika virus, is a simple method of controlling the number of babies who have microcephaly as a result of the virus. Unfortunately, although it is the simplest preventative measure, I do not think birth control is the most effective option considering the population that is affected. Many women have religious beliefs that are not in support of birth control and unfortunately safe sex practices are not necessarily always carried out by people in any country. Based on a Huffington Post article by Melissa Grant, the Pope has recently declared it permissible to take birth control due to the Zika crisis. Thus, factors such as this must be considered when thinking about preventative measures. Grant continues explaining that birth control is also not necessarily an easy expense for many rural, impoverished individuals. Brazil has now subsidized birth control to make it more accessible for the poor. If Zika virus became an issue in the United States, our poor would also be at the highest risk. Contrary to belief, birth control is not the most inexpensive, accessible drug, especially for the uninsured. Even Medicaid has certain stipulations for those uninsured and unable to afford health insurance on their own that can be a roadblock to these individuals being covered. Thus, will our government subsidize birth control like Brazil if Zika becomes an epidemic in the U.S.? Hopefully, this will not have to be a consideration.
http://www.huffingtonpost.com/melissa-s-grant/zika-virus-alters-catholic-church-policy-on-contraception_b_9301410.html#comments
I think the key to controlling this virus as cases begin to emerge in other countries, including the United States, lies with prevention and control methods while a vaccine is in development. Vaccines often take 10-15 years to produce from idea to product. There are many stages in which a vaccination must pass in order to make it to human trial. Vaccine Development Testing and Regulation The World Health Organization claims that though there are many organizations working on a vaccine, it that it will be at least 18 months before vaccines could be tested in large-scale trials.” Since the vaccine for Zika will likely take years to develop, I suggest epidemiologists and officials devise a concrete prevention and control plan.
Malaria has been an issue in endemic areas for thousands of years. Although the control method is not perfect, I believe we could model a new eradication method for arboviruses (both West Nile and Zika) based on prevention methods utilized for other diseases. Of course, those in endemic areas should continue control methods already in place, but I think more novel methods should be introduced. Although not very popular, I think the proposition to use DDT in endemic areas should be revisited since the effects of Zika disease in infants is such a chilling occurrence. With the help of the Gates foundation, I also believe the use of donated mosquito netting dipped in permethrin or DDT would be extremely helpful in South America. The Gates’ proposition to “give mosquitoes an STD” also seems promising…as predatory methods have been used for years to eradicate fly populations on rural farms.Gates Foundation| Mosquito Control
The WHO has several novel proposals for mosquito control including genetically modified versions of the Zika carrying, sneaky, “opportunistic,” aggressive, and hardy Aedes agypti mosquito vector. Although in the beginning stages of trials and approval, this method may not be as widely accepted by those affected heavily by the virus. Another idea, the release of a population of sexually sterile male mosquitoes can allow the breeding of mosquitoes, but no viable offspring, also seems to show potential as a new and effective method of mosquito control. Since mosquito eggs are hardier than other mosquito species, and the larva can essentially survive any temperature as long as they are in water, however, begs the issue that introducing a sterile male will not get rid of offspring that may lie dormant for some time. Thus, introducing a naturally occurring infection with Wolbachia bacterium will allow no hatching of mosquito offspring. Since this does not require genetic modification, it may be more widely accepted by locals and would be effective in reducing mosquito populations. WHO| Mosquito Control
As mosquito netting is being donated to these endemic areas, I also believe methods of contraception, like condoms, should also be donated to prevent the transmission from human male to female. The sexual transmission lifecycle of the virus makes this virus much more difficult to eradicate, as it now essentially has two reservoirs as opposed to one, but I believe with the right combination of prophylactic measures, viral spread can be reduced significantly until a vaccine is readily available.
I think the idea of genetically modified mosquitoes is interesting and could prove very useful with the right amount of caution and research. There is a proposal from Oxitec that suggests injecting lethal genes into eggs of Aedes aegypti mosquitoes. When the eggs hatch, they would then release a group of male mosquitoes into an environment that is at risk for Zika. This would allow the males that carry the lethal gene to mate with females that can transmit the virus, causing the overall mosquito population to be decreased in the area. The goal would eventually be to wipe out the entire species, as they transmit other diseases besides Zika.
Some argue there are plenty of benefits of this approach. The author argues that it is safer to let a species go extinct through genetic modification rather than introduce a new trait into the population because there could be more unexpected effects as a result. With extinction, the outcome is fairly guaranteed. Others have also pointed out that similar experiments have helped eradicate other pests, such as the screw worm.
However, the research needed for these programs are generally underfunded, especially in the United States. This could relate to the skeptical public opinion surrounding genetic modification. Some people are uncomfortable with controlling such things, and so it could be difficult to get the financial backing needed to adequately support this effort. In order for researchers to explore this viable option, it would be necessary to increase outreach programs to educate people on the benefits. Then, genetic modification may allow us to eventually wipe out populations of disease transmitting mosquitoes.
This is very interesting, thanks for the reply AColorless! I did not come across the use of the lethal eggs in my findings. I would like to make a comment however, that I found that areas that are endemic for many of these viruses (WNV, Zika, Ebola) and heavily affected by them, are usually third world populations that still heavily incorporate superstition into their daily lives. These populations are also the same that view genetic modification as unacceptable according to their values…so yes, I absolutely agree that public education of these populations will be necessary to rid these areas of the mosquitoes, and thus, the diseases. I think that it will however, not be an easy feat to persuade them from their religion and cultural values.
Though the Zika virus is quickly spreading, and has been moving in from South America, I feel this article over glorifies the virus. According to the CDC, there have been no reported fatalities linked to the Zika virus. In fact, the virus symptoms are very mild and affected individuals usually recover within a week. Symptoms include regular viral symptoms: muscle aches and fever. This virus becomes dangerous only when passed through a woman’s placenta to her fetus. Microcephaly occurs, which results in developmental delay, impaired motor skills, and speech impediments. there have been 4,000 reported cases of microcephaly in Brazil in neonates due to Zika since October 2015, compared to only 150 reported cases only 1 year prior.
Though vaccines are a great answer to aid in prevention, I think there should be more of an effort to create a drug therapy targeted towards pregnant woman infected with Zika virus, or pregnant women who have an increased risk of contracting the virus. The virus is not dangerous or fatal to non pregnant individuals. So creating a vaccine would only minimize minor suffering one has to endure for less than a week. However, a neonate contracting the virus suffers a limited lifespan, or a difficult and neurologically deficit lifestyle. A medication targeted towards pregnant women can prevent microcephaly, and would alleviate the suffering and difficulties an individual and his/her family would endure from neurological diseases.
For a pregnant woman with Zika virus, a vaccine will do her no good if the virus still crosses the placenta. I think more effort should be placed towards identifying the Zika virus pathway. Can a drug be created that will prevent the virus crossing the placenta? Is this even possible? I don’t know much about this. But this kind of targeted therapy would prevent the microcephaly caused by transmission of Zika virus to the fetus.
I feel this approach is economically savvy as well. In creating a vaccine, there would have to be a mass production of the drug, for a broad range of people to be able to access. However, the population of pregnant women is a smaller population. There would not have to be as many drugs manufactured, because the target is only for a more specific population. This would save government/tax payer time and money. At the end of the day, a vaccine would still be necessary. But, targeting the pregnant woman and her fetus seems to be a better approach.
I think the Zika virus can be just as serious in the normal adult population as the pregnant women population. Although Guillain-Barré syndrome in adults is not as common as microcephaly in newborns, it still cause permanent nerve damage and paralysis. The syndrome can weaken muscles and stop the ability to breathe on your own. According to the CDC one out of five cases have caused death.
I really think the United States are not alarmed by Zika because so far the only reported cases are traveled related, but the U.S. have a native aedes mosquito that can get the Zika virus and infect Americans. Once the aedes species mosquitoes are affected in the U.S., Americans can suffer just as greatly as South America and other places. Aside from Guillain-Barré syndrome, microcephaly in newborns can change the way Americans have children. If majority of pregnancies ended in a birth effect like microcephaly, then the human population as a whole will decline until a vaccine is created.
Every year we encounter a different strain of a virus, but as of 2015 the one that is causing the most problem is Zika virus. Zika virus spread by Aedes genus mosquito. These mosquitos like to bite during the day and love light colors. According to (WHO), this virus was first encountered in 1947 in West Africa, but it did not cause a lot of damage which leads me to believe that this strain that we are facing today is a mutant of the original one. This makes me think that if the government was to pass a law eliminating light colorful clothing that we will be able to slow down the virus infection being that the Aededs mosquitos are only active during the day. we can also create clothing with glass nanospheres so that when the mosquitoes’ senses someone the nanospheres will transmit amorous amount of light to the mosquitoes hindering it from biting the host. Another thing that we can try for now is making sure that we clean up and not leaving dirty water unattended to being that the mosquitoes loves those environments. As Anthony Fauci stated, “even with the production of a vaccine, it will be hard to determine how effective the vaccine is being that the symptoms only show up in 80% of the infected population”. I agree this virus is causing a major problem because of how fast it is spreading and if a vaccine is not produced anytime soon we are looking at a decline in the population and that is why regulation of clothing colors will really help.
Although the Zika infection is linked to microcephaly, according to the World Health Organization (WHO) it was never scientifically proven that microcephaly is actually a result from contracting the Zika virus. While patients who have given birth to in Brazil and the Caribbean’s have been exposed to the Zika virus and the infant born, was born with microcephaly, it may have been a cause of Craniosynostosism or even exposure to alcohol and drugs that will cause the baby brain to be abnormal.
In addition to the Zika virus being correlated with the cause of microcephaly in babies who mothers have been exposed to the Zika virus, it was also recently correlated with Guillain- Barre Syndrome (GBS). A study, that was the first of its kind, was conducted to find actual evidence that associated the Zika virus with GBS. The was able to positively correlate exposure to Zika with the appearance of GBS in individuals. From this study being conducted, hopefully scientists will be able to associate common immunological and endocrine dysfunctions and come up with a vaccine.
Thoughtful comments. Until recently, I was wholly inattentive to the rise of Zika, partly because I seldom watch the news, and partly because I have trouble taking care of myself as is. Two subtle events opened my eyes and allowed me to see that Zika is a global issue and one that must be addressed in all haste. The first thing was when my brother and his newly married wife deferred their honeymoon to Cancun, Mexico, because they were terrified of reports of Zika-related microcephaly. I feel like that fear is relatable and shared by many Americans, which leads me to consider the social and economic implications Zika virus presents as well. Social impact being adults hesitant to have kids or travel as much, economic impact being decreased tourism as examples. Clearly, I’m not an expert sociologist or economist, but common sense tells me Zika is really bad for both. Just today (July 22, 2016), several studies documented the growing number of abortion requests in Zika-stricken regions of Latin America, places where the procedure is already “illegal or highly restricted” (Aiken et al., 2016). That sadly leaves many pregnant women in those areas with little options. If and when Zika comes to the States, I can only wonder how it will affect our birth rate and our abortion rate if left unchecked. I admit I get bogged down in the statistics, and I realize microcephaly is the worst-case scenario for the children of Zika-infected pregnant women, still the thought that it could occur to you or someone you know or someone you don’t know—that truly scares the heck out of me. The second thing was when a public health official came to my house and gave me a door hanger that had information on West Nile Virus, another bug spread by mosquitoes, which can kill you and likewise has no cure. In short, I realized I know very little about these diseases, and it’s sparked an interest in me to learn more about tropical parasites in general. For me, and many others I assume, it starts with awareness and knowing the facts. I am looking forward to the trials and hoping we’ll able to prevent cases like these in the near future.
Aiken AR, Scott JG, Gomperts R, Trussell J, Worrell M, Aiken CE. Requests for Abortion in Latin America Related to Concern about Zika Virus Exposure. New England Journal of Medicine N Engl J Med. 2016. doi:10.1056/nejmc1605389.
Zika virus, a flaviviridae family virus has its provenance from Zika forests of Uganda. Until recently, a seemingly innocuous virus is now expeditiously spreading from Brazil to Carribean and parts of America by host Aedesv mosquito. According to the CDC, six cases of Zika virus related birth defects (microcephaly) have been reported in the US.
Despite the fact that there is no effective vaccine against Zika virus till date, vaccine scientists are moderately optimistic about vaccine boost against Zika virus in the coming future. Owing to the simplicity of its structure and similarity to other flaviviridae viruses make vaccine development efforts against Zika easier. It is crucial to know the protein code of the Zika in order to uncover its mode of action in host for an effective vaccine development. Scientists at Purdue University have partially been successful in decoding the protein map of Zika virus, and thus paving an avenue towards effective and safe vaccine production. Although vexed efforts have been invested for the development of Zika virus, its actual commercialization will take more time, and the hunt for effective vaccine development will continue in coming future.
I also think that the biggest challenge lies in diagnosing the case. Tests for Zika are not readily available and are relatively expensive too. Enhanced preparedness is our best bet at this moment to combat this emerging pandemic. Avoiding areas where Zika’s spreading, proper clothing, staying indoors, and use of mosquito repellents to avoid virus infection. Since the virus can be sexually transmitted, proper awareness needs to be raised among partners. Governments should act in unison and provide resources for accelerated R&D.
On July 26, 2016, the very first subject in a phase I trial by InovioPharmaceuticals, Inc. was given his/her first dose of the Zika DNA vaccine (GLS-5700). Earlier this week, the FDA approved a clinical trial for this experimental vaccine. (This is groundbreaking as the hunt for a vaccine for the Zika virus has become a top priority in the healthcare field.) “In preclinical testing, the vaccine induced robust antibody and T cell responses in small and large animal models.
According to an article on Stat , “GLS-5700 is a DNA vaccine” — DNA that is coded to produce the protein that surrounds the Zika virus is injected into the skin. Then a device that delivers an electrical pules is zapped at the site of injection. This electrical pulse helps the DNA gain entry into cells. This process is referred to as “electroporation.” Next, the cells will tells the immune system the Zika virus is invading and foreign, and antibodies will be produced against it.
Hopefully, GLS-5700 is successful. The Zika virus is rapidly spreading — becoming a sort of epidemic!
I think it’s so interesting that they developed a vaccine so quickly after the spread of Zika. Although, GLS-5700 has shown promise in antibody and T-cell responses, we have yet to see the side effects or the long-lasting effects of the vaccine. I am interested to know why the DNA vaccine therapy was never used for other mosquito related outbreaks such as West Nile Virus and perhaps Malaria? Is there pressure to find a vaccine because of the Rio Olympics and the press surrounding the safety of the athletes and visitors? In the mean time, since it will take time to develop a safe vaccine, people who are concerned and live in the areas where the disease is more prevalent should take preventative measures to keep mosquitoes away from them like keeping most of their body clothed, using insect repellent on exposed parts, using mosquito bed nets, and keeping homes cool.
One of the most challenging issues our societies are facing today stem from highly mutated viruses. As we have learned, Zika virus became known as early as 1947. However, it was not as prevalent as the incidences we see today. Considered by the World Health Organization as a pandemic, Zika has made appearances in several countries and has affected many thousands of people, most notably causing microcephaly-related disease in newborn infants. One can presume that, without a solution, these staggering statistics will only rise, which highlights the importance of our scientific community in finding a viable vaccine against the disease.
Currently, research is focused on investigation of existing vaccinations for other virus towards an eye on a possible extrapolation for a foundation for Zika virus. For instance, the DNA-based vaccine for West Nile virus, a live-attenuated vaccine for dengue virus, and an investigational vaccine developed for ebola virus have all been studied for compatibility with, and defense against, Zika virus.
One of the limitations in carrying out these above-mentioned investigations for development of a vaccine against Zika virus lies in the common practice of administering experimental vaccines initially on mice. Although the results can provide valuable information as to the possible effects on humans, a very different reaction may result when tested on humans. Testing can also be conducted on the carrier of the virus itself, which may produce more possibilities for a solution.
More evidence in support of the difficulty of developing an effective vaccine can be seen by the way the planned clinical trials of the vaccine prototype to be done in September 2016 on 80 patients are set up to only yield two results: 1) the vaccine’s safety and 2) its effectiveness. Eventually, once a viable formulation is created, further testing can be done to improve upon its usefulness, however, at that this time, the study is still in its primarily stages. It has been stated that even if this early testing is successful, a mass-marketed vaccine might not become available for many years.
Zika Virus is one of the main concerns in today’s society. Although the first case was reported in 1947 in West Africa, this virus became of an importance when the case started in Brazil. Now researchers are finding way to develop a vaccine for the virus. This interests me to see how long it will take to develop the virus. I know that different strains of the virus must be studied in order to develop the effective vaccination. Mosquito-borne illness such as malaria is a common disease in tropical areas such as India. Whenever I travel to India during the summer, my doctor would prescribe medication to protect myself from malaria. I am wondering if later on in the years when people will travel to places where the Zika virus is present people will get some kind of medication to protect themselves from the virus.
The Zika virus carriers, the Asian Tiger mosquito, are very actively during the day and can survive indoors and outdoors. The most interesting fact is that the Zika virus was discovered in monkeys in 1947 first, then the first human case occurred in 1954. Back then, medical technologies were not so advanced. Now in 2016, technologies have advanced and many researchers can actually study the virus more effectively. My only question is that I was learning in my medical microbiology class, a “new disease” is classified as a disease after 1976. My professor mentioned the Zika virus as a “new disease” so if the first case was reported in 1954, why is this a new disease?
Although vaccines may increase the overall immune response against the Zika virus, will the immune response be able to eradicate the viral infection before embryonic implantation? In my opinion with the Zika virus infection people and presenting passing symptoms it may not be as beneficial to work on a vaccine for a passing disease when the virus may present more alarming side-effects to a fetus. With further research found an article entitled “Zika Virus Infection during Pregnancy in Mice Causes Placental Damage and Fetal Demise”. This experiment was a researchers performed this to experiment to examine the infectious route utilized by the Zika virus. Results of the experimentation showed viral presence in a mouse embryo in as little as 7-8 days after infection. The virus was injected and in the paw of the mouse and able to attack placental cells to be able to enter and infect the embryo. While in utero the virus was then be able to infect and replicate in neural tissue to lead to microcephaly and fetal death. In this experiment the mice could be a model for human embryonic development and while not yet studied, I feel that the path when infection a pregnant human female. In my opinion I feel that some sort of gene therapy would be the most beneficial thing to do since the virus doesn’t have any long term effects on human adults that we know of at the moment.
Link to article